In recent years, the field of healthcare has witnessed a remarkable transformation with the becoming popular of Cell and Gene Therapy (CAGT). This innovative approach holds incredible pential for revolutionizing the way we treat complex diseases and disorders. By harnessing the power of genetics and cellular engineering, CAGT offers new avenues for targeted and personalized therapies.
🔗 In case you missed our last CAGT post 7 months ago, where we showcased how to find publications with Clinical Study Protocols, Statistical Analysis Plans, TLF shells for SAP, and full package of documentation for DMC attached, check it out here: TUNECT’s Insights on Oncology and Gene Therapy Design
So, what exactly is Cell and Gene Therapy?
Cell and Gene Therapy involves modifying or manipulating genes and living cells to address disease at its core. It encompasses a range of advanced therapeutic techniques that aim to:
✅ Replace disease-causing genes with healthy copies
✅ Inactivate malfunctioning genes
✅ Introduce new or modified genes to aid in disease treatment
![Gene Therapy: Types, Vectors [Viral and Non-Viral], Process, Applications and Limitations](https://tune-ct.com/wp-content/uploads/2023/07/new-baanner-.001-e1560763693164-300x160.jpeg) Gene Therapy: Types, Vectors [Viral and Non-Viral], Process, Applications and Limitations
Gene Therapy: Types, Vectors [Viral and Non-Viral], Process, Applications and Limitations
Cell Therapy
When it comes to cell therapy, there are two main types based on the origin of cells used: autologous and allogeneic cell therapies.

Autologous cell therapy involves using a patient’s own cells for treatment. The cells are harvested from the patient, modified or expanded in the laboratory, and then reintroduced back into the same patient. Since the cells are derived from the patient’s own body, there is usually no risk of rejection or immune response. Autologous cell therapy is commonly used in treatments such as chimeric antigen receptor (CAR) T-cell therapy for cancer.
On the other hand, allogeneic cell therapy involves using cells from a donor other than the patient. The donor cells are carefully matched to minimize the risk of immune rejection. Allogeneic cell therapy offers the advantage of using readily available donor cells, which can be modified and expanded to treat multiple patients. This approach is commonly used in treatments such as hematopoietic stem cell transplantation for certain blood disorders.
Introduction to Different Types of Cell Therapy:
- Human Embryonic Stem Cell (hESC) Therapy: Human embryonic stem cells are derived from embryos and have the ability to differentiate into various cell types. They hold great potential for regenerative medicine and tissue repair. However, their use raises ethical considerations due to the source of the cells.
- Induced Pluripotent Stem Cell (iPSC) Therapy: Induced pluripotent stem cells are adult cells that have been reprogrammed to an embryonic stem cell-like state. These cells have the ability to differentiate into various cell types and offer the advantage of being patient-specific, reducing the risk of immune rejection.
- Mesenchymal Stem Cell (MSC) Therapy: Mesenchymal stem cells are multipotent cells that can differentiate into various cell types, including bone, cartilage, and fat cells. They possess anti-inflammatory and immunomodulatory properties, making them useful in treating conditions such as autoimmune diseases and tissue injuries.
- Immunotherapy: Immunotherapy involves using cells of the immune system, such as T cells or natural killer cells, to target and eliminate cancer cells. This approach harnesses the body’s own immune system to fight against cancer and has shown promising results in certain types of cancers.
Each type of cell therapy has its unique advantages and considerations. Ongoing research and clinical trials are further exploring the potential of these therapies in addressing various diseases and conditions, paving the way for advancements in the field of regenerative medicine.
Gene-modified cell therapies have revolutionized the field of medicine by harnessing the power of genetic engineering to enhance the therapeutic potential of cells. Here are three prominent types of gene-modified cell therapies:
- CAR T-Cell Therapy (Chimeric Antigen Receptor T-Cell Therapy): CAR T-cell therapy involves modifying a patient’s own T cells to express a chimeric antigen receptor (CAR) on their surface. The CAR is designed to recognize specific antigens present on cancer cells. Once infused back into the patient, these genetically modified CAR T cells can selectively target and eliminate cancer cells. CAR T-cell therapy has shown remarkable success in treating certain types of blood cancers, such as leukemia and lymphoma.
- TCR (T-Cell Receptor) Therapy: TCR therapy aims to modify T cells to express T-cell receptors specific to cancer-associated antigens. TCRs are naturally occurring receptors on T cells that recognize specific antigens. By introducing engineered TCRs, T cells can be redirected to target cancer cells with precision. TCR therapy has shown promise in treating solid tumors, expanding the scope of gene-modified cell therapies beyond blood cancers.
- HSC (Hematopoietic Stem Cell) Gene Therapy: Hematopoietic stem cell gene therapy involves modifying hematopoietic stem cells, which are responsible for generating various blood cells. By introducing therapeutic genes into these stem cells, the modified cells can produce functional proteins or correct genetic mutations. HSC gene therapy holds potential for treating inherited genetic disorders, such as severe combined immunodeficiency (SCID), sickle cell disease, and certain types of muscular dystrophy.
Each of these gene-modified cell therapies offers a unique approach to tackling diseases by empowering the patient’s own cells with enhanced capabilities. They have demonstrated remarkable clinical outcomes and hold promise for the future of personalized and targeted medicine. Ongoing research and clinical trials continue to expand our understanding and application of gene-modified cell therapies in diverse disease areas.
Gene therapy is a rapidly evolving field that aims to treat or cure diseases by introducing genetic material into a patient’s cells. Here are three common types of gene therapy approaches:
- Adeno-Associated Viral (AAV) Vector Gene Therapy: AAV vectors are commonly used in gene therapy due to their ability to efficiently deliver genetic material to target cells. AAV vectors are derived from a non-pathogenic virus called adeno-associated virus. In this approach, the therapeutic gene is inserted into the AAV vector, which is then introduced into the patient’s cells. AAV-based gene therapy is often used for gene augmentation or replacement, where the therapeutic gene is added to supplement the function of a defective or missing gene.
- Adenoviral Vector Gene Therapy: Adenoviral vectors are derived from adenoviruses, which are common viruses that cause respiratory infections. Adenoviral vectors have high gene transfer efficiency and can accommodate large genetic payloads. They are particularly useful for delivering genes to target cells in various tissues. Adenoviral vector gene therapy can be employed for gene augmentation, replacement, or even cancer therapy by delivering therapeutic genes that target tumor cells.
- CRISPR-Cas9 Gene Editing: CRISPR-Cas9 is a revolutionary gene editing technology that has transformed the field of genetic engineering. It utilizes a guide RNA (gRNA) to direct the Cas9 enzyme to a specific target sequence in the genome. Once at the target site, Cas9 creates a double-stranded break in the DNA, allowing for precise modification of the genetic material. CRISPR-Cas9 gene therapy enables genome editing, which involves modifying specific genes by either introducing desired changes or repairing genetic mutations.
Method of Action in gene therapy can employ different mechanisms to achieve therapeutic effects:
- Gene Augmentation/Replacement: This approach involves introducing a functional copy of a gene into the patient’s cells to supplement or replace a defective gene. By providing the correct genetic instructions, the therapy aims to restore normal cellular function and alleviate disease symptoms.
- Genome Editing: Gene therapy utilizing genome editing techniques, such as CRISPR-Cas9, aims to modify specific genes within the patient’s genome. This can involve correcting disease-causing mutations, disrupting harmful genes, or introducing precise genetic changes to achieve therapeutic outcomes.
RNA therapeutics offer a promising approach to treat diseases by targeting specific nucleic acids or proteins within cells. Here are four common types of RNA therapeutics:
- Antisense Oligonucleotides (ASOs): ASOs are short synthetic nucleic acid sequences designed to bind to specific RNA targets. By binding to the target RNA, ASOs can modulate gene expression by altering RNA splicing, promoting RNA degradation, or inhibiting RNA translation. ASOs can target a wide range of nucleic acid targets, including messenger RNA (mRNA) and non-coding RNA, and they hold potential for treating genetic disorders, neurodegenerative diseases, and certain types of cancers.
- Small Interfering RNA (siRNA): siRNA molecules are double-stranded RNA molecules that can selectively degrade specific mRNA molecules within cells. By targeting mRNA, siRNA therapeutics can inhibit the translation of disease-associated genes, effectively reducing the production of disease-causing proteins. siRNA therapeutics have shown promise in treating various conditions, including viral infections, genetic disorders, and certain types of cancers.
- Aptamers: Aptamers are short, single-stranded nucleic acid sequences that can bind to specific target molecules with high affinity and specificity. They can be designed to target various types of molecules, including proteins, small molecules, and even cells. Aptamers can interfere with protein-protein interactions, block protein function, or act as carriers for therapeutic molecules. Due to their versatility, aptamers have potential applications in diagnostics, targeted therapy, and drug delivery.
- Messenger RNA (mRNA): mRNA therapeutics involve the direct administration of synthetic mRNA molecules into cells to provide instructions for the production of therapeutic proteins. By delivering exogenous mRNA, this approach aims to compensate for deficient or malfunctioning proteins in the body. mRNA therapeutics have gained significant attention recently, particularly with the development of COVID-19 vaccines using mRNA technology. They hold promise for treating a wide range of diseases, including genetic disorders, cancer immunotherapy, and regenerative medicine.
Method of Action of RNA therapeutics exert their effects through different mechanisms, depending on the specific type and target:
- Nucleic Acid Targets: ASOs, siRNAs, and some aptamers primarily target nucleic acids, such as mRNA or non-coding RNA. By binding to specific sequences on these nucleic acids, RNA therapeutics can modulate gene expression, either by promoting the degradation of targeted RNA or by blocking translation processes.
- Protein Targets: Aptamers and certain siRNAs can target specific proteins directly. Aptamers bind to proteins with high affinity, inhibiting their activity or interfering with protein-protein interactions. Similarly, siRNAs can specifically degrade mRNA molecules encoding disease-associated proteins, leading to reduced protein levels.
- Protein Encoders: mRNA therapeutics act as carriers of genetic information to encode specific proteins within cells. Synthetic mRNA molecules are delivered to cells, where they are translated into therapeutic proteins, compensating for deficiencies or introducing desired protein functions.
How does it work?
 What is Gene Therapy? and How Does it Work?
What is Gene Therapy? and How Does it Work?
Gene therapy involves altering the genetic code within a person’s cells to treat or cure diseases. This can be achieved through various mechanisms, such as replacing or repairing defective genes, or turning off genes that are causing problems. By doing so, gene therapy holds the promise of addressing the underlying causes of diseases rather than just managing their symptoms.
On the other hand, cell therapy utilizes living cells to restore or enhance the function of damaged tissues or organs. These cells can be sourced from the patient (autologous) or from other donors (allogeneic). Cell therapy approaches include immune cell therapies, cancer vaccines, and the use of stem cells for therapeutic purposes.
Promising Applications of CAGT
The potential applications of CAGT are vast and continue to expand. Researchers are exploring the use of cell and gene therapies in treating a wide range of diseases, including:
🔬 Cancer: Gene therapies show promise in targeting cancer cells specifically, offering potential alternatives to conventional treatments like chemotherapy.
🔬 Genetic Disorders: CAGT holds the potential to address inherited genetic conditions by targeting and modifying the underlying genetic mutations responsible for these disorders.
🔬 Infectious Diseases: Gene therapies can be utilized to enhance the body’s immune response and combat infectious diseases, offering novel treatment approaches.
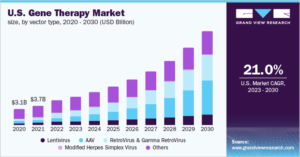 Gene Therapy Market Size, Share & Growth Report, 2030
Gene Therapy Market Size, Share & Growth Report, 2030
Regulation and Safety
Cell and Gene Therapy products are subject to rigorous regulation and oversight to ensure their safety and efficacy. In the United States, the Food and Drug Administration’s Center for Biologics Evaluation and Research (CBER) oversees the regulation of cellular therapy products, gene therapy products, and related devices. Clinical studies undergo thorough evaluation to assess safety and effectiveness before products can be approved for use in humans.
🔗 To learn more about CAGT and its regulatory framework, visit the FDA’s Cellular & Gene Therapy Products page.
🔗 The European Medicines Agency (EMA) also provides valuable information on Advanced Therapy Medicinal Products (ATMPs), including gene and cell therapies.
Pushing the Boundaries of Medicine
Cell and Gene Therapy are at the forefront of cutting-edge medical research. These innovative treatment modalities have the potential to transform the lives of patients by targeting diseases at their genetic roots. As scientists and healthcare professionals continue to push the boundaries of what is possible, we eagerly anticipate the breakthroughs and advancements that lie ahead.
🌐 Stay informed about the latest developments in Cell and Gene Therapy by exploring resources such as ClinicalTrials.gov and PubMed for scientific publications.
🌐 Follow leading organizations and research institutions dedicated to CAGT, including the National Institutes of Health (NIH) and International Society for Cell & Gene Therapy (ISCT), to stay updated on the latest news and advancements.
Together, we can witness the transformative potential of Cell and Gene Therapy as it continues to shape the future of healthcare. Let’s embrace this exciting frontier and work towards a world where personalized, targeted treatments offer hope and healing to those in need.

